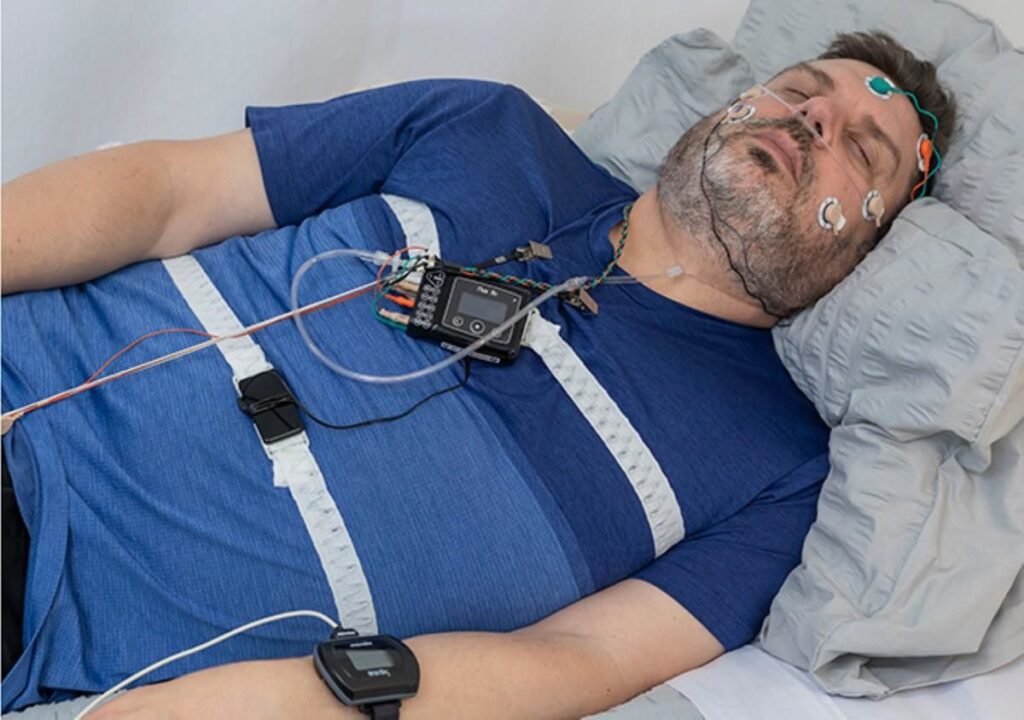
This guide breaks down what Medicare usually covers for sleep apnoea testing, what it typically does not, and the easiest ways to avoid surprise costs.
What does Medicare usually cover for a sleep apnoea test?
A sleep apnea test medicare benefit is generally available when the test is considered medically necessary and is ordered under Medicare-approved guidelines. In most cases, coverage applies when a doctor evaluates symptoms, documents the medical need, and refers the patient for an appropriate sleep study.
Coverage for a sleep apnea test medicare claim may vary depending on whether the study is performed in a sleep clinic (in-lab test) or conducted at home, as well as the provider’s billing practices and Medicare participation status.
Who is eligible for Medicare-covered sleep apnoea testing?
They are usually eligible if a doctor believes they have signs or symptoms consistent with sleep apnoea and the test is medically necessary. Common triggers include loud snoring, witnessed pauses in breathing, choking or gasping during sleep, excessive daytime sleepiness, and high blood pressure that is hard to control.
Medicare is not designed to pay simply because someone is curious about their sleep quality. The referral and documentation matter.
Which symptoms and risk factors make Medicare coverage more likely?
Medicare coverage is more likely when symptoms are clear and persistent, and when risk factors increase the likelihood of obstructive sleep apnoea. These often include obesity, a large neck circumference, older age, male sex, family history, nasal obstruction, and certain jaw or airway shapes.
Co-existing conditions can strengthen the case, such as atrial fibrillation, resistant hypertension, type 2 diabetes, stroke history, and heart failure, where untreated sleep apnoea may worsen outcomes.
What types of sleep apnoea tests can Medicare cover?
Medicare can cover different kinds of sleep studies depending on clinical need and what the referring doctor requests. The two main categories are:
- In-lab polysomnography (PSG): A comprehensive overnight study in a sleep lab.
- Home sleep apnoea testing (HSAT): A simplified study performed at home with portable monitoring equipment.
The “best” option depends on their symptoms, medical complexity, and whether a home test is appropriate.
Is an at-home sleep apnoea test covered by Medicare?
Often, yes, if it is ordered appropriately and performed through a Medicare-eligible provider. Home testing is commonly used when obstructive sleep apnoea is strongly suspected and there are no complicating medical factors that require an in-lab study.
However, home tests are not always suitable. If they have significant heart or lung disease, suspected central sleep apnoea, or other complex sleep disorders, Medicare-funded pathways may lean towards in-lab testing instead.
Is an in-lab sleep study covered by Medicare?
In many cases, yes, when the test is medically necessary and meets Medicare requirements. In-lab studies are more detailed and can be essential when the diagnosis is unclear, symptoms are severe, or there is concern about conditions beyond straightforward obstructive sleep apnoea.
In-lab studies can cost more than home tests, so understanding billing and any gap fees is crucial before booking.
What does Medicare typically not cover for sleep apnoea testing?
Medicare typically does not cover testing that is not clinically justified, not properly referred, or provided outside eligible arrangements. Common situations that can lead to little or no Medicare support include:
- Screening tests without documented symptoms or medical need
- Consumer “sleep tests” sold directly to the public
- Add-on services marketed as wellness upgrades rather than clinical necessities
- Testing arranged through providers who do not bill Medicare for that service
Even when Medicare covers part of the test, it may not cover the full cost.
Will Medicare cover the entire cost, or are there out-of-pocket gaps?
Medicare does not automatically mean “free”. They may still face out-of-pocket costs depending on whether the provider bulk bills, charges a gap, or bills above the Medicare Schedule fee.
They should ask for a written quote before proceeding. A quick phone call can prevent a large bill later, especially with private sleep clinics.
Does Medicare cover sleep apnoea testing through a GP, specialist, or both?
Medicare coverage usually starts with a GP assessment and referral, but some pathways involve a sleep physician or respiratory specialist. The key issue is not just who refers them, but whether the referral and test meet Medicare rules and are billed correctly.
If their case is complex, a specialist assessment may improve the chance they are sent to the right test first time, which can reduce repeat testing and extra fees.
Other Resources : Assessment of General Practice Experience
What steps should they take to maximise Medicare coverage and avoid surprises?
They should treat this like any other medical procedure: confirm eligibility, confirm billing, and confirm what is included. A practical checklist is:
- Ask the referring doctor what test is being ordered and why
- Confirm the provider is Medicare-eligible for that service
- Ask whether the test is bulk billed or has a gap
- Request a written estimate that lists all fees
- Clarify whether a follow-up appointment is billed separately
- Keep copies of the referral and any symptom questionnaires
Small admin steps can save hundreds of pounds.
What questions should they ask the sleep clinic before booking?
They should ask direct, specific questions that force clear answers. For example:
- “Do they bulk bill this sleep study under Medicare?”
- “If not, what is the expected gap, and what is included in that fee?”
- “Does the quote include equipment, scoring, reporting, and clinician interpretation?”
- “Are there separate fees for set-up, consumables, or follow-up?”
- “If the home test is inconclusive, what happens next and what would it cost?”
If a clinic cannot explain costs clearly, that is a red flag.
Does Medicare cover repeat sleep studies or retesting?
Sometimes, yes, but it depends on medical need. Retesting may be appropriate if the first study was inconclusive, symptoms persist despite treatment, significant weight changes occur, or treatment settings need reassessment.
They should not assume repeat testing is automatically covered. The medical justification and the exact billing item used can change what Medicare pays.
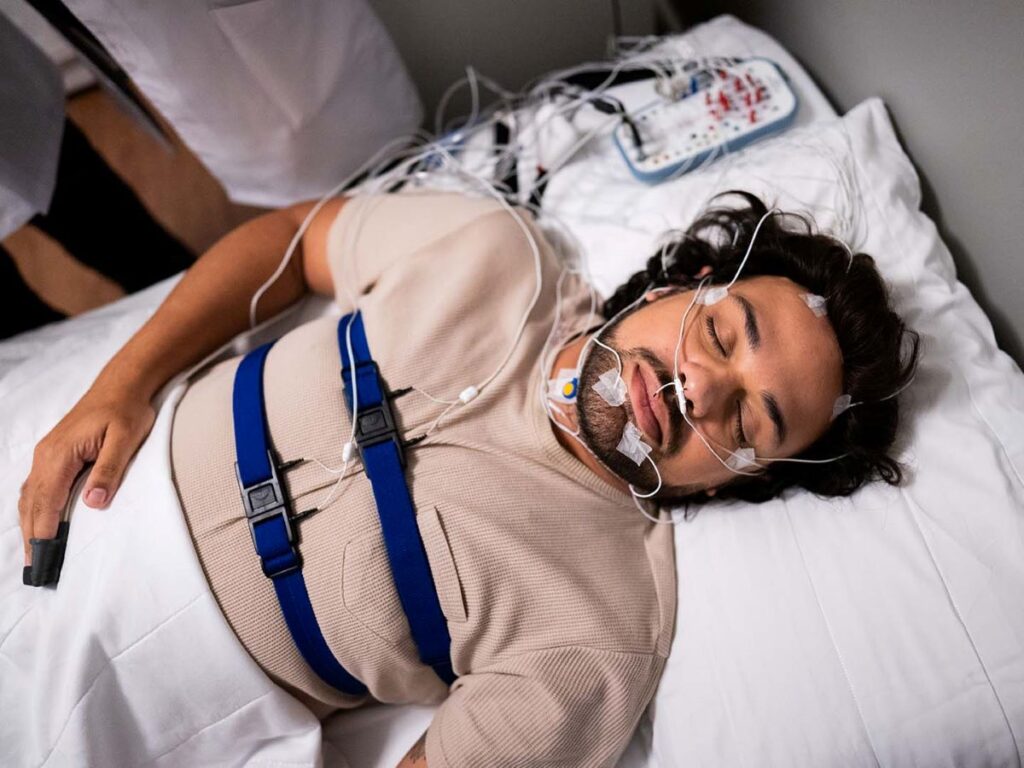
Is treatment covered too, or only the test?
The test is only one part of the journey. Medicare may support certain consultations and follow-ups, but many common treatment costs, especially equipment, can involve out-of-pocket payments.
For example, CPAP machines and accessories are often purchased privately, although some people may access assistance through private health insurance, state programmes, or other support pathways depending on circumstances. Click here to get more about sleep test Brisbane: what to expect before, during and after.
What’s the simplest way to think about Medicare coverage for sleep apnoea tests?
Medicare coverage is most likely when the test is clearly medically necessary, properly referred, and provided by a clinic that bills Medicare correctly. It is least likely when testing is treated like a wellness product or arranged outside standard clinical pathways.
If they focus on documentation, eligibility, and upfront fee checks, they can usually get the testing they need without financial surprises.
FAQs (Frequently Asked Questions)
What does Medicare usually cover for sleep apnoea testing?
Medicare generally covers clinically necessary sleep studies when ordered and performed under correct Medicare-eligible arrangements. This includes tests referred by a doctor who has assessed symptoms and documented medical need. Coverage varies depending on whether the test is done in a sleep clinic (in-lab study) or at home (home sleep test), and on the provider’s billing practices.
Who is eligible for Medicare-covered sleep apnoea testing?
Eligibility for Medicare-covered sleep apnoea testing typically requires a doctor to identify signs or symptoms consistent with sleep apnoea and deem the test medically necessary. Common indicators include loud snoring, witnessed breathing pauses, choking or gasping during sleep, excessive daytime sleepiness, and difficult-to-control high blood pressure. Medicare does not cover tests requested solely out of curiosity about sleep quality.
Are at-home sleep apnoea tests covered by Medicare?
Yes, often they are covered if ordered appropriately and performed through a Medicare-eligible provider. Home sleep apnoea testing (HSAT) is commonly used when obstructive sleep apnoea is strongly suspected without complicating medical factors. However, home tests may not be suitable for those with significant heart or lung disease, suspected central sleep apnoea, or other complex conditions, where in-lab studies may be preferred.
Does Medicare cover in-lab sleep studies for diagnosing sleep apnoea?
In many cases, yes. In-lab polysomnography (PSG) is covered when medically necessary and meeting Medicare requirements. These comprehensive overnight studies are essential for unclear diagnoses, severe symptoms, or concerns beyond straightforward obstructive sleep apnoea. Since in-lab studies can be more expensive than home tests, understanding billing and potential gap fees beforehand is important.
What costs might not be covered by Medicare during sleep apnoea testing?
Medicare typically does not cover tests that lack clinical justification, proper referral, or are provided outside eligible arrangements. This includes screening without documented symptoms, consumer-directed ‘sleep tests’, add-on wellness services rather than clinical necessities, and services from providers who do not bill Medicare. Even when partially covered, patients may face out-of-pocket costs depending on billing practices.
How can patients maximise Medicare coverage and avoid unexpected costs for sleep apnoea testing?
Patients should confirm eligibility and billing details before proceeding: ask the referring doctor about the test type and reason; ensure the provider is Medicare-eligible; check if the test is bulk billed or involves a gap fee; request a written estimate covering all fees including equipment and reporting; clarify if follow-up appointments incur separate charges; and keep copies of referrals and symptom documentation. These steps help prevent surprise expenses.