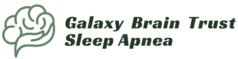This guide explains what they can expect before, during, and after a sleep study, including common prep steps, what the night looks like, and how results usually work.
What is a sleep test, and why would they need one?
A sleep test Brisbane measures breathing, oxygen levels, heart rate, sleep stages, and body movements while they sleep. It is commonly used to investigate snoring, choking or gasping at night, morning headaches, poor concentration, and daytime sleepiness.
It can also support diagnosis of conditions such as obstructive sleep apnoea, central sleep apnoea, periodic limb movement disorder, and some insomnia-related patterns.
What types of sleep tests are available in Brisbane?
Most people are offered either an at-home sleep test or an in-clinic overnight study. The best option depends on symptoms, health history, and what the doctor needs to rule in or out.
Home studies are often used when obstructive sleep apnoea is strongly suspected. In-lab studies are more comprehensive and may be recommended if symptoms are complex or if other sleep disorders are possible.
How do they get referred and booked in?
They usually start with a GP appointment, where symptoms, medical history, and risk factors are reviewed. If a sleep study is appropriate, the GP may refer them to a sleep specialist or directly to a sleep testing provider, depending on the pathway.
Booking times vary. They may be asked a few screening questions, complete forms, and confirm whether the test is at home or at a clinic.
What should they do in the week before the test?
They should follow the instructions provided by the clinic or provider, because requirements can differ by test type. In general, they will get the best results by keeping sleep habits as normal as possible.
They may be asked to avoid major schedule changes, and to share a list of medicines and supplements. If they use sleeping tablets, nasal sprays, or recreational substances, they should disclose this rather than guessing what to stop.
What should they avoid on the day of the sleep test?
They are commonly advised to avoid caffeine later in the day and to skip alcohol, because both can alter sleep architecture and breathing. Naps are often discouraged, especially in the afternoon, as they can reduce sleep drive overnight.
They should also avoid heavy meals close to bedtime if reflux or snoring is a concern. If they are unsure, they should follow the provider’s written instructions over general advice.
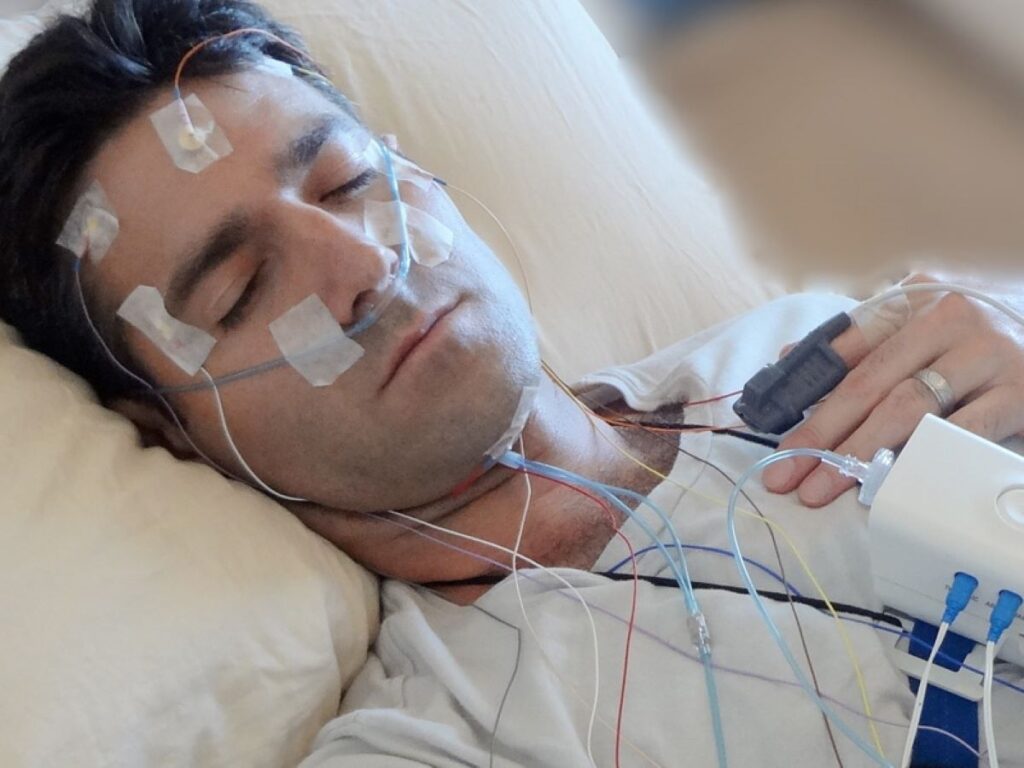
What happens during a home sleep test in Brisbane?
A home sleep test usually involves a small recording device and a few sensors they apply before bed. Common sensors include a finger probe for oxygen, belts around the chest or abdomen for breathing effort, and a nasal cannula to measure airflow.
They sleep in their own bed and return the device the next day. The goal is to capture typical sleep in a familiar environment, with minimal disruption.
What happens during an in-clinic overnight sleep study?
An in-clinic study (often called polysomnography) is conducted in a sleep lab designed to feel like a quiet bedroom. A technician attaches sensors to the scalp, face, chest, and legs to record brain waves, eye movements, muscle activity, breathing, and oxygen levels.
They can usually bring personal sleep items, such as pyjamas and a pillow. A technician monitors signals from another room and can assist if sensors loosen overnight.
Will the sensors hurt or stop them from sleeping?
The sensors should not be painful, but they can feel unfamiliar. Some people sleep less than usual, and that is expected. Sleep clinicians can often still interpret results even if sleep is lighter or broken.
If they worry they will not sleep at all, they should mention it beforehand. Providers can explain how much recorded sleep is typically sufficient for analysis.
What should they bring or prepare for the night?
For home testing, they may only need comfortable sleepwear and a simple plan for fitting the device correctly. For an in-lab study, they should bring toiletries, any medicines they take at night or early morning, and something to wear to bed.
They should also wash their hair and avoid heavy hair products if scalp sensors are used. Clean, product-free skin helps electrodes stick and improves signal quality.
What happens after the test is finished?
After a home study, they return the equipment as instructed, often the next business day. After an in-lab study, sensors are removed in the morning and they can usually leave soon after.
They may feel slightly tired if sleep was disrupted. Most people can return to normal activities the same day, unless their clinician has advised otherwise.
How long do results take, and what do they usually include?
Results commonly take several days to a couple of weeks, depending on provider capacity and whether specialist review is required. The report typically summarises breathing events, oxygen drops, snoring patterns, sleep stages, and overall sleep efficiency.
For suspected sleep apnoea, the report often includes an index of breathing interruptions per hour and how severe they are. Their doctor uses this alongside symptoms to decide next steps.
What treatment options might follow a positive result?
If obstructive sleep apnoea is diagnosed, common options include CPAP therapy, mandibular advancement splints, weight management support, positional therapy, and addressing nasal obstruction. The right plan depends on severity, anatomy, and tolerance.
Some people need further testing, such as CPAP titration or additional sleep studies, especially if symptoms do not match the first result.
What questions should they ask their GP or sleep specialist afterwards?
They should ask what the diagnosis is, how severe it is, and how it explains their symptoms. It also helps to ask what treatment is most effective for their level of severity and what success looks like.
If CPAP is recommended, they can ask about trial periods, mask fitting, comfort settings, follow-up schedule, and how adherence is monitored and supported.
How can they make the sleep test as accurate as possible?
They should aim for a typical night: normal bedtime, usual sleeping position, and standard routine where possible. They should apply sensors carefully for home tests and contact the provider if something seems wrong rather than guessing.
Most importantly, they should provide honest information about alcohol, medicines, and sleep habits. Accurate context makes interpretation more reliable and recommendations more personalised.
Related : Sleep Apnea Test Medicare: What’s Covered and What’s Not?
FAQs (Frequently Asked Questions)
What is the purpose of a sleep test in Brisbane and who should consider taking one?
A sleep test in Brisbane helps clinicians understand reasons behind snoring, exhaustion, or breathing interruptions during sleep. It records key signals overnight so a GP or sleep specialist can diagnose conditions like obstructive sleep apnoea and recommend appropriate treatment. It’s commonly suggested for those experiencing symptoms such as loud snoring, choking or gasping at night, morning headaches, poor concentration, or daytime sleepiness.
What types of sleep tests are available in Brisbane and how do I know which one is right for me?
In Brisbane, there are two main types of sleep tests: at-home sleep tests and in-clinic overnight studies. Home tests are often used when obstructive sleep apnoea is strongly suspected, offering convenience by allowing you to sleep in your own bed with minimal disruption. In-clinic studies (polysomnography) are more comprehensive and recommended for complex symptoms or other possible sleep disorders. The choice depends on your symptoms, health history, and your doctor’s recommendation.
How should I prepare in the week leading up to my sleep test?
Preparation varies depending on the type of sleep test but generally includes maintaining normal sleep habits without major schedule changes. You should provide a list of all medicines and supplements you’re taking, including sleeping tablets, nasal sprays, or recreational substances—disclosing these is important rather than guessing what to stop. Following any specific instructions from your clinic or provider will help ensure accurate results.
What can I expect during an overnight in-clinic sleep study in Brisbane?
During an in-clinic overnight study, conducted in a quiet bedroom-like lab, a technician attaches sensors to your scalp, face, chest, and legs to monitor brain waves, eye movements, muscle activity, breathing patterns, and oxygen levels. You can bring personal items like pyjamas and pillows to feel comfortable. A technician monitors the recordings from another room and assists if sensors loosen during the night.
Will wearing sensors during the sleep test be uncomfortable or affect my ability to sleep?
The sensors used in both home and in-clinic tests should not cause pain but may feel unfamiliar. Some people experience lighter or broken sleep during the test night; this is expected and clinicians can usually interpret results despite this. If you’re concerned about not sleeping at all during the test, inform your provider beforehand—they can explain how much recorded sleep is typically sufficient for analysis.
How long does it take to receive results from a sleep test in Brisbane and what happens next?
Results typically take several days to a couple of weeks depending on provider capacity and whether specialist review is needed. The report summarises breathing events, oxygen levels, snoring patterns, sleep stages, and overall efficiency. For suspected obstructive sleep apnoea, it includes an index of breathing interruptions per hour with severity grading. Your doctor will use this information alongside your symptoms to decide on next steps such as treatment options or further testing.